Hidradenitis Suppurativa: Early Recognition, IL-17 Targeted Therapies, and Multidisciplinary Care
Clinical Summary
Hidradenitis Suppurativa (HS): Early Recognition, IL-17 Therapies, and Multidisciplinary Care
-
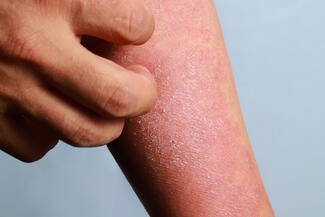
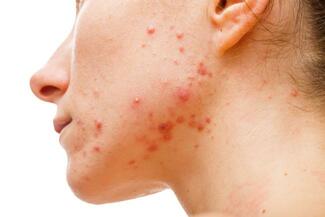
Early diagnosis (HS; ~10-year delay): Prioritize recurrent abscesses/boils in intertriginous areas (axilla, inframammary, groin, buttocks), history of “folliculitis,” recurrent colorectal abscess care, and association with nodulocystic acne; increase awareness among ER, PCP, OB-GYN.
-
Therapeutic landscape (biologics): Beyond TNF-α inhibitors, IL-17A and IL-17A/F inhibitors expand options; selection depends on disease phenotype, prior treatment, and comorbidities (e.g., inflammatory bowel disease, arthritis).
-
Multidisciplinary management: Essential due to comorbidities (metabolic syndrome, type 2 diabetes, cardiovascular risk); dermatologists should screen and coordinate care with primary care, OB-GYN, and mental health to optimize long-term outcomes.
Reviewed by Riya Gandhi, MA, Associate Editor of Immunology Group
Dr Jack O’Brien discusses how dermatologists can reduce diagnostic delays in hidradenitis suppurativa by recognizing early clinical signs such as recurrent abscesses in intertriginous areas and associated acne. Learn how IL-17A and IL-17F inhibitors are expanding treatment beyond TNF-α therapies and why multidisciplinary care—integrating primary care, OB/GYN, and mental health—is essential to improve long-term outcomes in HS patients.
Transcript
Hi, I'm Jack O'Brien. I'm an assistant professor of dermatology at UT Southwestern Medical Center in Dallas, Texas. I'm the director of our hidradenitis suppurativa clinic and focus on medical and surgical management hidradenitis suppurativa as well as clinical trials.
With diagnostic delays in HS averaging nearly a decade, what early clinical signs or patient cues should dermatology providers be prioritizing to improve timely recognition?
Dr O'Brien: I think there's a couple things that I would think of the dermatologist should prioritize in terms of early recognition of HS. I think obviously if a patient has recurrent abscesses, boils, may report history of folliculitis in intertriginous areas, the axilla under the breast, the groin, the buttock area, they should be suspicious of hidradenitis suppurativa. I think the other consideration certainly is also if the patient mentions seeing colorectal surgery for recurrent abscesses, might be relevant to screen for HS. I think patients with severe acne, nodular cystic acne who might be candidates for isotretinoin, often that can go along with hidradenitis suppurativa so good to screen them.
I think the final thing the dermatologist really can do to help with earlier detection and screening of HS is educating their local community. The ER, the primary care doctors who refer to them, OB-GYN providers. I think a lot of education of the local community to raise awareness for HS is also very important because often the patient's first point of contact with HS, their first point of contact with the medical community is usually the ER, their primary care doctor, or their OB- GYN.
How are emerging therapies—particularly those targeting IL-17A and IL-17F—shaping the treatment landscape beyond TNF-α inhibition, and what do clinicians need to know when choosing among these agents?
Dr O'Brien: I think it's a very exciting time to be treating hidradenitis suppurativa because of all of the newer therapeutic options that we have for patients beyond TNF alpha inhibition. I think often the considerations that I make when I'm determining which biologic is the best option for treating a patient with hidradenitis suppurativa depends somewhat on their treatment history, the specific phenotype of their disease and the other comorbid conditions that they might have. For example, if the patient has inflammatory bowel disease, typically it's TNF inhibitor is often a better option or factoring in whether or not they have arthritis and things like that. But it's a really exciting time to have multiple other options, including IL-17A and IL-17A/F inhibitors for treatment of patients with HS.
What role does multidisciplinary care play in optimizing long-term outcomes for HS patients, and how can dermatology practices better coordinate with other specialties like OB/GYN, mental health, and primary care?
Dr O'Brien: I think multidisciplinary care for patients with HS is not optional. I think it really is mandatory and it is critical in order to optimize the long-term management of patients with HS. I think we know that HS is associated with multiple other comorbid conditions, including metabolic syndrome and up to 50%, type 2 diabetes, and increased cardiac events, among many other comorbid conditions. And I think it's very important as dermatologists to be aware of these associations, to screen for them, and to ensure the patient has follow up with the appropriate providers, whether that's their primary care doctor, mental health providers, OB- GYN. I think oftentimes patients may think that as they may not have a primary care doctor and they may see you as a dermatologist, you may be checking some blood work for lab monitoring, and the patient may assume that you are kind of managing all of the things that they need to be managed for. And so as a dermatologist, it's really important to develop those collaborations with physicians because you may be the patient's main point of contact with the medical system and helping them be screened for the other conditions that go along that we know are associated with HS is important to optimize the long-term management of patients.