Systemic Sclerosis: Emerging Treatments
Clinical Summary
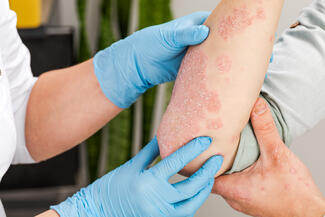
Systemic Sclerosis (SSc): Emerging Therapies and Multidisciplinary Management
-
CAR-T therapy (autoimmune SSc, early studies): Targeted B-cell depletion shows potential for deep remission; current trials enroll late-stage, treatment-refractory patients. Optimism centers on earlier intervention for disease modification.
-
Targeted immunomodulators & antifibrotics: SSc involves immune activation, vascular dysfunction (Raynaud’s, PAH, ulcers), and fibrosis (skin, lung). Multiple agents in clinical trials target discrete pathways; precision medicine likely needed rather than one-size-fits-all therapy.
-
Practical care considerations: Multidisciplinary coordination is essential; patients often require multi-drug regimens, increasing interaction and infection risk. Balance organ-specific benefit with cumulative immunosuppression.
Reviewed by Riya Gandhi, MA, Associate Editor of Immunology Group
Dr Scott Elman discusses emerging advances in systemic sclerosis, including targeted immunomodulators, antifibrotic agents, and the potential role of CAR-T therapy in disease modification. Learn how precision medicine, earlier intervention, and multidisciplinary collaboration may reshape long-term outcomes in SSc while balancing safety and organ-specific management.
Scott Elman, MD, FAAD, is an assistant professor of dermatology in the Dr Phillip Frost Department of Dermatology & Cutaneous Surgery at the University of Miami Miller School of Medicine, who also serves as the director of inpatient dermatology services at the University of Miami Hospital.
Transcript
Hi, I'm Dr Scott Elman. I'm an internist and dermatologist. I practice at the University of Miami Department of Dermatology. I'm thrilled to be here at Masterclasses of Dermatology, my favorite meeting of the year.
With systemic sclerosis carrying high morbidity and mortality, what recent advances give you the most optimism for changing its long-term trajectory?
Dr Elman: Systemic sclerosis is one of my favorite conditions to treat because it has such a severe impact on patient quality of life, and it really can be devastating. The challenge with systemic sclerosis is that there's multiple domains, multiple organs that could be impacted. And screening for these is important. We want to make sure that we're taking comprehensive care of our patients, but treating this is really difficult as well because in my experience and the lived experience of those who care for these patients, it's not a one size fits all treatment. Things that work for treating the skin don't necessarily work for treating the lungs and vice versa.
And so it gives me hope, what gives me excitement is there are a lot of new drugs coming to treat systemic sclerosis. If you go search clinical trials for systemic sclerosis, it is overwhelming. And there's a lot of excitement. Still, one of the challenges is that many of the drugs in development are only looking at maybe a small snapshot of systemic sclerosis. Things are being studied for the lungs. Things are being studied for the vascular kind of component of this, whether it be Raynodes or ulcers, and also a subset of drugs are being looked at for skin sclerosis specifically. The thing that I'm most excited for, although I think that it's excitement with a little bit of tempered optimism is CAR-T therapy. There's been a lot of buzz around this as a form of potential treatment disease modification of our autoimmune connective tissue diseases, systemic sclerosis, lupus, idiopathic inflammatory myopathy. And there's a lot of excitement buzz about deeper clinical remission by very clearly and swiftly and ninja-like targeting B-cells.
The challenge remains though, because currently these studies are being done almost like a last line. Folks are really at the end stage of their disease. They failed everything. And I'm a little nervous that they might not work in this late stage. I think where there's a lot of optimism, what I'm hopeful for is earlier intervention will lead to earlier success in this. And so that's where I think we need to head, although we're still a little bit far away from it.
How are emerging targeted immunomodulators and antifibrotic agents reshaping our understanding of disease modification in SSc?
Dr Elman: In general, the pathogenesis of systemic sclerosis is a little bit tricky because it's not just one thing that goes wrong. There's this immune inflammatory cascade that happens that triggers two distinct things. So we've got issues with vascular. So there's vascular dysfunction that happens and that contributes to a lot of the pathogenesis that we see of Raynodes, of pulmonary arterial hypertension, of wounds and ulcers. And then we have fibrosis, kind of a different pathway, maybe late stage of that vascular inflammation that really leads to the skin thickening and to the pulmonary fibrosis as well. We understand this and we can target it, but we still have ways to go in terms of seeing success here. So I'm optimistic that targeting these pathways will lead to benefit, but that's also what we've been doing for a while as well. So my hope is with more specific molecules, hitting different pathways, maybe one of these things will pan out.
When I lecture, when I think about the pathogenesis of systemic sclerosis, it is overwhelming. I mean, there's a lot involved here. This is not psoriasis where one molecule can be targeted to lead to complete clearance. This is one where I think it's going to take some time to figure out what is the right medicine for which patient. And I think the future of systemic sclerosis is going to be some form of precision medicine of figuring out which patient needs what, but the more medicines that we have approved to treat this, the smarter we're going to look and the better we're going to be able to treat our patients.
What practical considerations should dermatologists keep in mind when incorporating newer or regenerative therapies into multidisciplinary SSc care?
Dr Elman: So practically, when we manage our patients with systemic sclerosis, of course, dermatologists play a significant role because we are likely the ones who are first diagnosing these patients, maybe not, but I think for a lot of these patients, dermatologists are the first shop that patients are coming to, but they're often not the last one. And as we think about managing these patients, of course, we have our organ, the skin, it's important. There's no doubt about that, but we really do have to think about what other organs are involved and we have to share. And so the issue that I find is that many patients with systemic sclerosis to attain good disease control, it requires being on multiple different therapies, and sometimes one hand doesn't talk to the other from different specialists. So we really need that multidisciplinary collaboration to take good care for these patients.
We have to be thoughtful that each one of our medicines is being used for a good reason, and at the same time, we want to make sure that we're minimizing interactions, but also minimizing immunosuppression if we can get away with it. Many of these patients end up on heavy hitter, heavy duty medications, and infection remains a real risk for them.