What Lies Beneath: Three Distinct Cases of Heel Melanoma
Heel melanoma is uncommon, but its location on a weight-bearing surface makes it easy to miss. These three plantar heel cases underscore how delayed recognition can lead to invasive disease and nodal spread, while timely biopsy and coordinated oncology care can improve outcomes.
Key Takeaways
- Timely biopsy is key. In these cases, lesions persisted from 2 months to 2 years and included ulceration/hypergranulation—features that can masquerade as neuropathic ulcers or chronic fissures. If a heel lesion is atypical, pigmented, changing, or fails to heal as expected, biopsy should move up the algorithm.
- Heel melanoma may already be invasive and node-positive at diagnosis. Two of 3 cases had positive sentinel lymph nodes, reinforcing that acral/plantar presentations can carry higher diagnostic delay and worse prognosis—making early recognition and staging critical.
- Multidisciplinary management works—and surveillance matters. All patients underwent wide local excision with sentinel node biopsy and adjuvant systemic therapy when indicated (eg, pembrolizumab), with healed wounds and no reported recurrence at follow-up—highlighting the value of coordinated podiatry, surgical oncology, and medical oncology pathways.
Melanoma, a highly aggressive and deadly form of skin cancer, can occur in uncommon locations such as the foot, accounting for 3–5% of all melanoma cases.1 Its high mortality rate, driven by delayed diagnosis, is a significant concern, with approximately 73,000 new cases and 10,000 deaths annually in the United States. The 5-year survival rate for advanced-stage melanoma is significantly reduced, emphasizing the need for early detection and treatment.2
This analysis examines 3 cases of plantar heel melanoma to highlight diagnostic challenges, treatment strategies, and the importance of timely intervention. By analyzing clinical presentation, management, and outcomes, this case series aims to enhance awareness among healthcare professionals and the public about melanoma of the foot and its unique features and diagnostic complexities. According to the National Cancer Institute, the incidence of melanoma has been increasing over the past few decades, with a projected 2% annual increase in new cases. Furthermore, a study published in the Journal of the American Academy of Dermatology found that melanoma of the foot is more common in individuals with darker skin tones, highlighting the need for targeted awareness and education campaigns across a broad scope of patients.3
The plantar heel, a weight-bearing area prone to trauma and chronic wounds, presents a unique challenge for early detection and correct diagnosis of cancer. Acral melanoma, a subtype of melanoma occurring on the palms, soles, and nail beds, is particularly rare and aggressive, accounting for approximately 1–3% of all melanoma cases in Caucasians, but up to 70% of cases in individuals with darker skin tones. Acral melanoma is often associated with a poorer prognosis due to its tendency to metastasize to lymph nodes and other distant sites.4
Invasive melanoma, characterized by its rapid growth and potential for metastasis, poses a significant threat to patient outcomes. The 5-year survival rate for invasive melanoma in later stages is approximately 30%, compared to 99% for in situ melanoma. If left untreated, invasive melanoma can metastasize to lymph nodes, lungs, brain, and other distant sites, resulting in a significantly poorer prognosis. Overall, the prognosis for patients with melanoma metastasized to the lymph nodes is generally poor, with a 5-year survival rate declining even further.5
In this case series of plantar heel melanoma, we highlight diagnostic challenges, treatment strategies, and patient-centered care considerations, with the goal of informing and enhancing management strategies for this aggressive condition.
Case #1
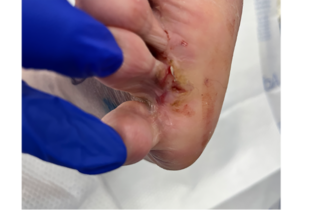
A 44-year-old Caucasian male presented to the podiatry clinic with a 2-year history of right heel pain. His past medical history was significant for hypertension and lumbar radiculopathy, with a family history of colon cancer, and without a personal smoking history. This lesion of the right plantar heel persisted for over 2 years with intermittent pain and fissuring.
Physical examination revealed a dark purple macule on the right plantar heel with asymmetry, irregular borders, ulceration, and crusting measuring 2.2 cm x 1.0 cm (Figure 1). Punch biopsy confirmed a diagnosis of invasive melanoma.
The patient then saw a surgical oncologist, who performed wide excision of the lesion and a sentinel lymph node biopsy, which was positive. Magnetic resonance imaging (MRI) of the brain was negative for metastasis, but computed tomography (CT) of the chest, abdomen, and pelvis revealed paraoesophageal lymphadenopathy. Oncology began pembrolizumab at a dose of 200 mg every 3 weeks for 1 year. Currently, the patient has completed treatment, his foot remains healed, with no apparent recurrence, and will continue under routine surveillance.
Case #2
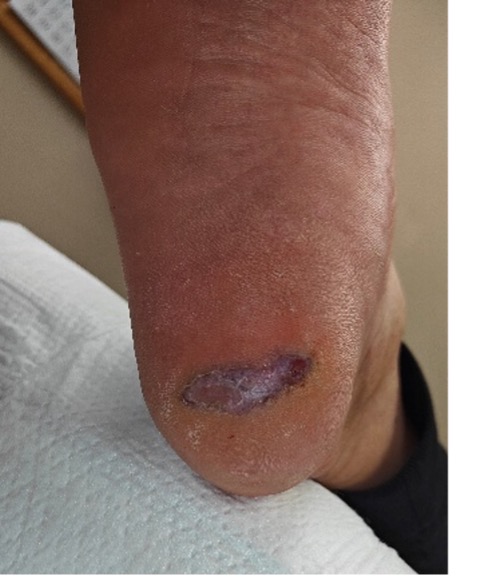
A 70-year-old Hispanic male with past medical history of alcohol dependence and idiopathic neuropathy presented with a chief complaint of chronic left heel ulcer. Physical examination revealed an irregularly bordered ulceration with a hypergranular wound base (Figure 2). Initial treatment included sharp debridement, silver-impregnated dressings, and an offloading shoe for wound healing. After months of nonhealing with standard of care, a 4-mm punch biopsy confirmed an invasive acral melanoma.
In this case, the surgical oncologist performed a wide local excision with sentinel node biopsy, which revealed a positive femoral sentinel lymph node. Cranial MRI and positron emission tomography (PET) were negative for distant metastasis. The patient received pembrolizumab at a dose of 200 mg every 3 weeks for 1 year. Approximately 2 years post-diagnosis, there are no signs of recurrence, and the patient continues to follow up for routine surveillance.
Case #3
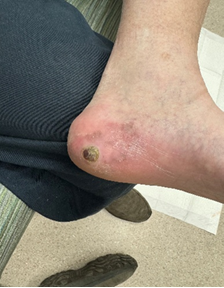
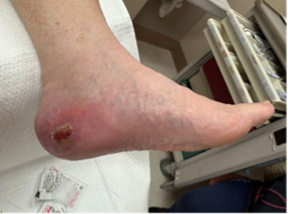
A 74-year-old Caucasian male with type 2 diabetes, sleep apnea, hypertension, hyperlipemia, and benign prostatic hyperplasia presented with a chief concern of a painful lesion to the left medial heel for 2 months. After attempting self-care by shaving down the mass, he decided to pursue medical care. Upon clinical examination, the lesion measured 1.0 x 1.0 cm, and appeared as a crusted and raised hyperpigmented papule painful to palpation.There was concern for malignancy due to the mass location (Figure 3). A 4-mm punch biopsy resulted in a diagnosis of malignant melanoma.
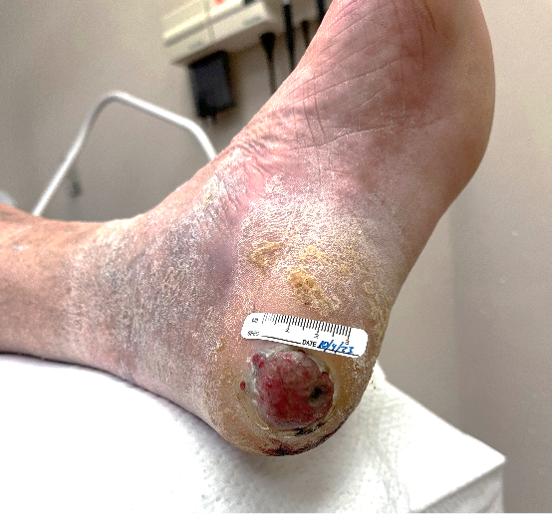
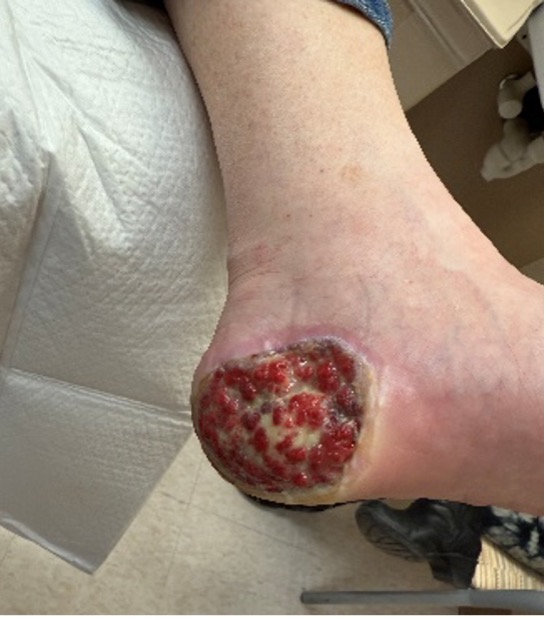
At this time the patient also saw surgical oncology for wide excision of the mass and sentinel lymph node biopsy, which was negative. The surgical excision resulted in a full-thickness wound (Figures 4, 5) for which the patient completed his wound care in the VA clinic and underwent chemotherapy for 1 year. As of the time of publication, the wound is healed with no recurrence.
Conclusion
Clinicians must maintain a high index of suspicion for melanomas when evaluating patients with persistent or chronic skin lesions, particularly those that fail to progress adequately toward healing. This is especially critical for lesions in atypical locations, such as the heel, where melanoma may be subtly presented but with aggressive potential. These cases of heel melanoma highlight the importance of early recognition to improve patient outcomes. Prompt biopsy combined with coordinated multidisciplinary care is essential for effectively managing acral and invasive melanoma subtypes. These subtypes, though uncommon, demand heightened clinical vigilance due to their potential for rapid progression and severe consequences. By acting judiciously and ensuring timely intervention, clinicians can significantly enhance outcomes through early detection and comprehensive treatment strategies tailored to the unique challenges of this serious condition.
Drs. Jacobson and Towson are third-year residents at Southern Arizona Veterans Administration Health Care System (SAVAHCS).
Drs. Walters and Samoy are Attending Podiatric Surgeons at SAVAHCS.
Dr. Dancho is the Chief of Podiatric Surgery at SAVAHCS.
References
- Rashid OM, Schaum JC, Wolfe LG, et al. Prognostic variables and surgical management of foot melanoma: review of a 25-year institutional experience. ISRN Dermatol. 2011;2011:384729. doi:10.5402/2011/384729
- American Cancer Society. Cancer Facts & Figures 2022. American Cancer Society; 2022.
- National Cancer Institute. Melanoma—Cancer Stat Facts. National Cancer Institute. Published 2022. Accessed March 13, 2026. https://seer.cancer.gov/statfacts/html/melan.html
- Nadelmann ER, Singh AK, Abbruzzese M, Adeuyan OO, et al. Acral melanoma in skin of color: current insights and future directions—a narrative review. Cancers (Basel). 2025;17(3):468. doi:10.3390/cancers17030468
- Heistein JB, Acharya U, Mukkamalla SKR. Malignant melanoma. In: StatPearls. StatPearls Publishing; 2025. Updated February 17, 2024. Accessed March 13, 2026. https://www.ncbi.nlm.nih.gov/books/NBK470409/
© 2026 HMP Global. All Rights Reserved.
Any views and opinions expressed are those of the author(s) and/or participants and do not necessarily reflect the views, policy, or position of Podiatry Today or HMP Global, their employees, and affiliates.