Improving Dermatology Measures for Skin of Color and Underrepresented Groups
Clinical Summary
Dermatologic Outcome Measures in Skin of Color: Limitations and Equity Strategies
-
Outcome measure limitations (e.g., EASI, SCORAD): Many dermatology studies do not report race, ethnicity, or skin tone, limiting generalizability. Reliance on Fitzpatrick skin type as a proxy oversimplifies skin tone variation and may misclassify disease severity.
-
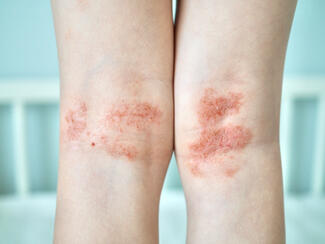
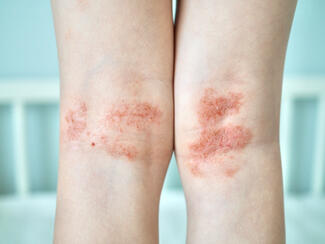
Measurement bias in darker skin: Scoring systems that rely on erythema assessment may underscore disease severity in darker skin tones; outcomes such as dyspigmentation, xerosis, and “ashiness” are often excluded despite clinical relevance.
-
Equity strategies for trials and practice: Validate scoring tools across diverse populations; adopt objective skin tone measures (e.g., Monk Scale, UMelanin scale, colorimeters); increase community engagement and trial enrollment, with targets of ~40% diverse participation by 2030.
Reviewed by Riya Gandhi, MA, Associate Editor of Immunology Group
This interview examines the limitations of commonly used dermatology outcome measures in patients with skin of color and other underrepresented populations. Dr Asempa discusses practical frameworks for developing more inclusive, skin-type-relevant assessment tools and shares strategies dermatologists can use to advocate for equitable endpoints in clinical trials and in everyday practice.
Transcript
Hi, I'm Oyatawa Asempa. I'm an assistant professor of dermatology at Baylor College of Medicine, and I direct the skin of color clinic there.
What are the key limitations of current dermatologic outcome measures when applied to patients with skin of color or from underrepresented groups?
Dr Asempa: So there are a lot of limitations. I think the first thing that comes to mind is a lot of studies or data sets don't even report race, ethnicity, skin tone. So it's hard to know whether or not the outcomes of these studies are generalizable to different populations. And when they do report race and ethnicity, they often use very simplistic, I like to say race proxies, things like Fitzpatrick. We've gotten used to seeing, but it doesn't adequately explain or even represent skin tones. It flattens an entire group of people as though if someone is one Fitzpatrick, that means a specific skin tone.
And so I think these are some of the key limiting factors in some of our scoring systems as well. So we can take the easy score or SCORAD and eczema, for example. Erythema is really important for these scores and people don't always see erythema in darker skin tones. And so we may be underscoring our darker skin tone patients with this. Some of the suggestions for how to fix that is just adding a score for anyone with darker skin, but that also has not been validated.
And I think the last limitation that I think about is not including outcome measures for things that affect patients of skin of color differently. For example, dyspigmentation is not frequently considered as an outcome measure or xerosis or ashiness, I like to say, is not always considered as an outcome measure. And these are the things that may affect darker skin tone patients more significantly.
What strategies or frameworks can help clinicians and researchers develop more inclusive, skin-type-relevant tools for measuring treatment outcomes?
Dr Asempa: I think the most important thing is to ground our outcome measures in the patient experience. That will automatically help us to be more inclusive in how we think about what's important when you look at outcome measures in research. But some specific things are validating the scores that we do have across different patient populations to know whether or not they truly are generalizable. And then really working on developing some more objective measures of skin tone that we use frequently in research. So instead of using Fitzpatrick in research, considering things like the monk scale or the UMelanin skin tone scale, different things that are more objective, using colorimeters in studies to know exactly, again, an objective measure of skin tone as opposed to using race as a proxy for skin tone.
How can dermatologists advocate for and implement more equitable outcome measures in both clinical trials and everyday practice?
Dr Asempa: I think the biggest things are we really do need to increase enrollment of diverse patient populations in clinical trials. There are a few ways that we can do this. One is more community involvement. I think that when you're in the communities teaching and educating, then you build trust in communities and communities are more likely to want to be involved in the research process. But then another thing is, even as individual dermatologists, wherever you practice, thinking about what clinical trials are going on in your area and then considering your patients, all of your patients, but especially your patients of color, and recommending them to these clinical trials, normalizing studies, normalizing research, helping to, again, build trust in the community. We really need to get our clinical trial representation to look like what our country looks like. And so there have been recommendations to try to get to 40% enrollment by 2030. So I think we have some work to do.